For those who are considering giving birth at the University of Tokyo Hospital.
We are here to help you have a safe delivery and will work closely with you to make the process as comfortable as possible.
Birth Plan
Doctors, midwives, and all medical staff work together to provide support for a safe and comfortable delivery. We provide continuous midwifery care from pregnancy to postpartum, including midwife-led motherhood classes and breastfeeding classes. We value each individual’s birth plan.
Semi-open system
For your convenience, we have adopted a semi-open system that allows you to receive a prenatal checkup at a nearby affiliated medical facility. You can choose a medical facility with easy access from several options to reduce waiting time for medical treatment. In the event of a suspected maternal or fetal disease or sudden change in condition at the collaborating medical facility, the University of Tokyo Hospital will take care of your case.
Advanced medical facilities and team medical care
As a comprehensive perinatal medical center, we have the medical facilities to safely deliver babies in high-risk pregnancies with maternal or fetal diseases, and provide team medical care in cooperation with obstetrics and gynecology, such as pediatrics, pediatric surgery, anesthesiology, radiology, internal medicine, surgery, and psychiatry etc.
| Facility | Obstetrics 30 general beds, 9 MFICU beds, 21 NICU beds, 36 GCU beds, 12 PICU beds. |
|---|
-
MFICU (Intensive Care Unit for Maternal-Fetal and Neonatal Medicine)
The MFICU is available for high-risk mothers and fetuses.
The room is equipped with delivery monitoring system, respiratory and circulatory monitors, ultrasound, ventilators, and dedicated staff to protect the mother and child around the clock. -
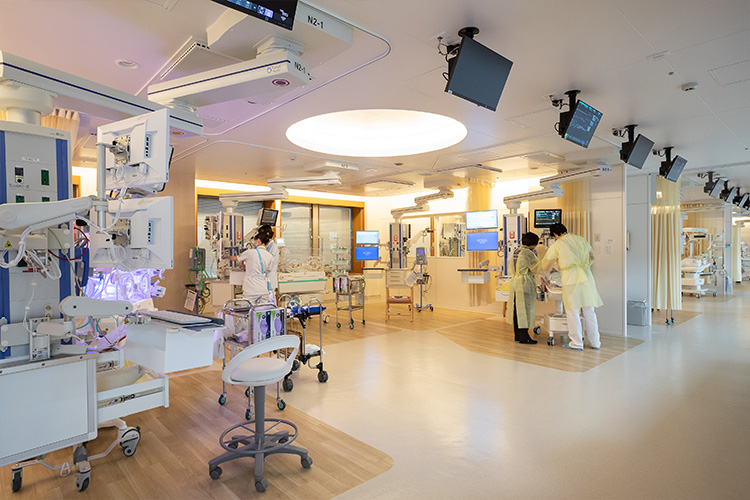
NICU・GCU (in the Children’s Medical Center)
The NICU/GCU is an intensive care unit for newborns who require special medical care, such as premature births, low birth weight babies, and babies born with heart problems. It is equipped with incubators to maintain sufficient body temperature, ventilators, and monitors to closely evaluate the body condition.

Delivery results
Elderly childbirth
Results in 2024
Over 35 years old: 504 cases (262 first births), 54.9% of the total births
Over 40 years old: 190 cases (94 first births), 20.6% of the total births
Multiple births
In 2024, the number of multifetal-pregnancy after 22 weeks was 36 cases of twins and 0 case of triplets, 0 case of monochorionic-monoamniotic twins (MM twins), 13 cases of monochorionic-diamniotic twins (MD twins), 23 cases of dichorionic-diamniotic twins (DD twins)
TOLAC
At our hospital, TOLAC (trial of labor after cesarean section) is limited to cases where the obstetrician and gynecologist determine that the conditions for a safe trial are met for those who wish to have a vaginal delivery after cesarean section.
Placenta previa and low-lying placenta
There were 36 cases of placenta previa/low-lying placenta in 2020. When placenta accreta or heavy bleeding is expected, we place a catheter for occlusion in the internal iliac artery before the cesarean section, making every effort to reduce the amount of bleeding. Caesarean section can be performed in a special operating room (hybrid operating room) where surgery and endovascular catheter treatment can be performed simultaneously.
Pregnancy with maternal diseases
Uterine and adnexal diseases (laparoscopic surgery during pregnancy for ovarian cysts, adenomyosis, management of pregnancies complicated by gynecological malignancies, etc.), thyroid diseases, psychiatric disorders, central nervous system diseases, respiratory diseases, autoimmune diseases, hemic diseases, cardiovascular diseases, infections, Rh Incompatibility During Pregnancy, treatments of infertility, etc.
Pregnancy with fetal disease
We can treat all congenital heart diseases that require medication or surgery, all diseases that require pediatric medical treatment, and all other diseases diagnosed during the fetal period, such as central nervous system diseases, renal and urinary system diseases, and bone system diseases.
External version
We perform pelvic exenteration for patients with breech pregnancies at 36-37 weeks. This operation includes moving the fetal head downward while anesthetizing the pelvic position. We will evaluate the condition of the mother and fetus to see if the operation can be performed safely. We will perform the procedure only after the sufficient explanation and with your consent.